Psychedelics offer genuine hope for better mental health. But they’re controversial. And they won’t heal every person with a mental health issue. Still, I believe there’s plenty to be excited about.
At any point in time, approximately 20 percent of adults have mental health issues that impact their ability to get or hold a job, maintain healthy relationships, or practice adequate self-care. At times of widespread stress, like a global pandemic, this percentage can surge much higher.
Despite this tsunami of need, mental health funding isn’t adequate and practitioners are overwhelmed. And that means that medication is usually the first—often only—line of treatment. Too often, medication alone doesn’t work, especially for conditions like PTSD, grief, or personality issues.
We urgently need new treatment options which are safe and effective.
How Psychedelics Can Help
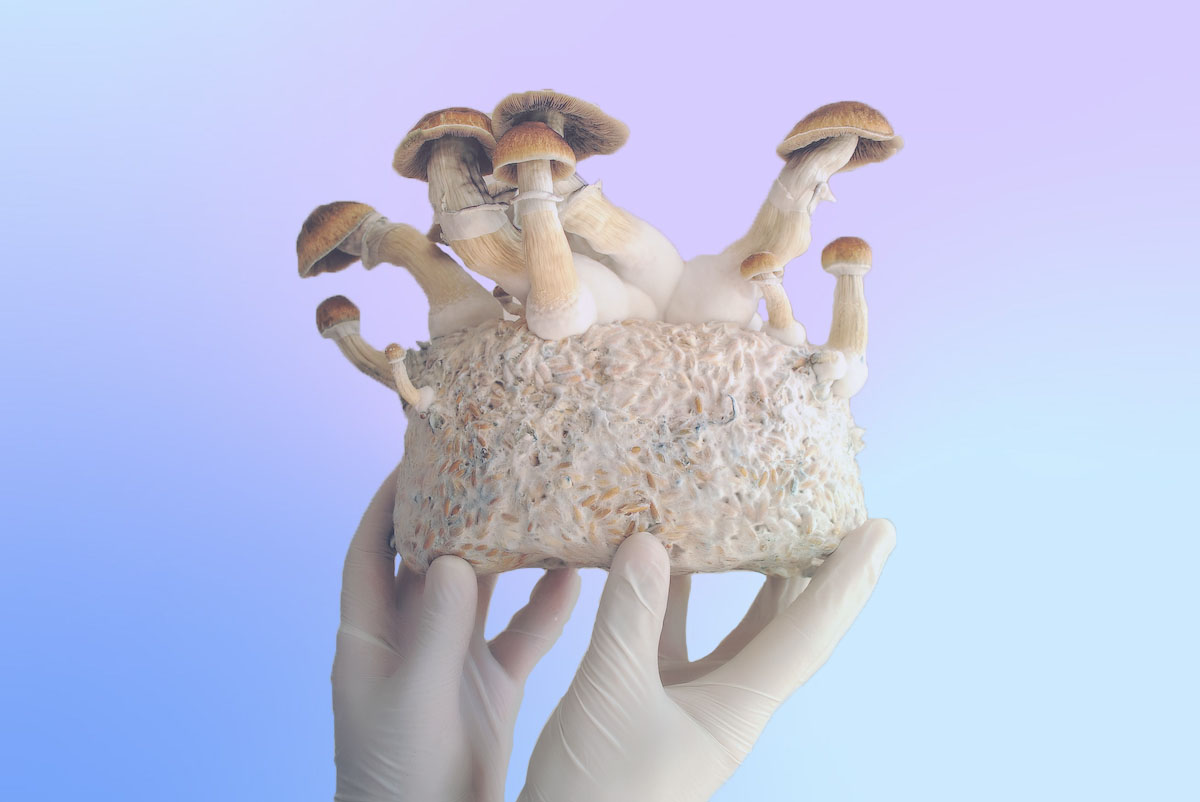
The combination of psychedelics plus new therapy approaches may be the most dramatic treatment breakthrough in mental health for decades.
When certain psychedelics are given along with the right type of psychotherapy, we can help those with a range of mental health problems. Psychedelic-assisted psychotherapy promises to revolutionize the treatment of mental health disorders.
All psychedelics are not the same. Different psychedelics cause different effects, lasting for variable periods of time, and each carries a different level of risk. And not every psychedelic will be useful with therapy.
The Psychedelic Compounds to Watch
In my new book, The Promise of Psychedelics, I rate and rank these psychedelics as wannabes, contenders, and as bronze-, silver-, and gold-medal champions. (In the book you’ll also learn why I believe that within five years psychedelics will become standard treatment, in combination with appropriate therapy, for many mental health conditions.)
Most psychedelic compounds pose too many risks and hold unproven benefits. Only a few can be considered for use in psychedelic-assisted psychotherapy.
Bronze Medal Winner: MDMA
There’s exciting data from clinical studies suggesting that in treatment-resistant patients with PTSD, MDMA can be useful as part of psychedelic-assisted psychotherapy. It’s also possible that MDMA may turn out to be useful in treatment for depression, anxiety, addictions, and eating disorders. There’s more work to do but some of the data already available is exciting.
MDMA is often considered a safe drug, but it’s not. It can cause dehydration, hyperthermia (high body temperature), restlessness, sweating, increased heart rate and blood pressure, and even kidney damage. MDMA itself can also cause depression. Other risk factors appear to rule out longer-term use.
This is why MDMA is likely to become part of a psychedelic-assisted therapy option only for treatment-resistant patients with a few major conditions.
Silver Medal Winner: Ketamine
Ketamine is a breakthrough product. The scientific evidence is strong that ketamine can rapidly benefit many patients who have depression, including those who don’t respond to medication treatment. Unlike drugs traditionally used to treat depression, where patients often wait weeks for signs of clinical benefit, ketamine can act within hours of its first use and it can last a few weeks.
There is also evidence that ketamine may be helpful in treating other conditions and it is being studied in many areas. However, ketamine—historically used as an anesthetic—is dangerous when used in unsupervised ways. It can cause neurological and cognitive issues, brain damage, and even death.
Gold Medal Winner: Psilocin
You’re likely more familiar with psilocybin (from magic mushrooms). When psilocybin is swallowed, the stomach and small intestine break it down into psilocin, and that’s the active metabolite that causes the psychedelic and hallucinogenic experiences. Psilocin is the compound actually responsible for the clinical benefits.
The structure of psilocin is similar to that of serotonin, one of the main reasons there’s so much exciting potential. As well as all the neurotransmitter and receptor impacts, there’s increasing evidence that psilocin increases nerve growth (neurosynthesis) and nerve connections by helping with development of new synapses (synaptogenesis). It may also increase the strength of connections between nerves.
This is why psilocin may help so many individuals overcome the effects of long-term mental health issues—by reversing nerve changes.
The Promise of Psychedelics
Many questions remain unanswered, including who is most likely to benefit from each psychedelic, how we can upgrade the psychotherapy to better match each one, and how to get access to the right psychedelics so the right patient can be paired with the right psychotherapy approach.
I believe psychedelics represent incredible potential—but not for casual use. Which is why I’ve never used psychedelics, and don’t plan to. My goal is to help those who have significant mental health issues, and I don’t need to try psychedelics to research the benefits.
Dr. Peter Silverstone is a psychiatrist, researcher, and founder and CEO of Zylorion Health. To learn more about psychedelics and the promise they bring, read Dr. Peter Silverstone’s forthcoming book from Ingenium Books, The Promise of Psychedelics: Science-Based Hope for Better Mental Health.



