This article was originally written by Third Wave, a platform that inspires cultural awakening through personal transformation.
After years of depressive spells, Caroline wondered if psychedelics could create the shift she needed. So she decided to try ketamine therapy. During the experiences, Caroline felt overwhelming peace wash over her. In between therapy sessions, she integrated the lessons with her guide. After four journeys, she felt empowered to observe her thoughts and feelings without spiraling out of control. Ketamine assisted therapy helped create the shift Caroline needed to find peace in her life; a form of mental health treatment that wouldn’t have been readily available to her just a few years ago. This invites the question: what can modern medicine stand to learn from Caroline’s experience.
Missing Elements
Caroline’s experience aligns with that of countless people who have overcome issues ranging from treatment-resistant depression to PTSD and addiction. Real-world insights like hers are critical to advancing the field of psychedelic medicine. At the same time, her compelling experience is one anecdote in a sea of unlinked stories about the beneficial use of psychedelic drugs. To give them credence, the medical community is realizing the urgent need for a system of universal best practices for psychedelic care, which do not exist today.
Without those standards, providers may not know how to manage risks and deliver the most beneficial treatment to the greatest number of people possible. Lack of measures could also limit safe access in clinical settings and ultimately cause society’s growing acceptance of psychedelics to regress. Until we bridge that gap, psychedelic therapy will remain on the fringe of mainstream medicine.
So, how do we ensure a future of sanctioned, accessible and scalable psychedelic therapy treatments? By spreading the word about its potential, garnering real-world insights from practitioners and participants, and incorporating the critical missing element–shared aggregate and anonymized data–to provide people with access to safe, tested, and proven care.
We Need to Recognize the Potential of Psychedelic Therapy
First, it is critical for health providers and society at large to recognize the wide-reaching therapeutic potential of psychoactive drugs. It’s also important to understand that “psychedelic therapy” does not imply a single-serve approach. It encompasses a far-reaching list of classic psychedelics and non-traditional hallucinogens that differ in their origins, effects, serotonin modulation, and uses. The most common psychedelics that induce self-healing through altered states of consciousness include the substances you see below.
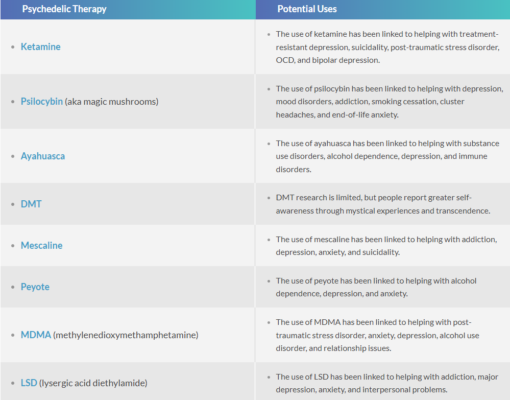
The field of psychopharmacology includes a breadth of psychedelic research and randomized controlled trials. It’s up to advocates to spread the word.

Understanding Psychedelic Research
A growing array of placebo-controlled, FDA-approved, double-blind trials exists alongside observational reports and clinical research across various psychedelic substances. Health professionals, practitioners, and patients can draw upon these insights–they just need to know the research exists.
Fortunately, an increasing number of well-known psychedelic proponents like Tim Ferriss and New York Times best-selling author Michael Pollan are committed to bringing psychedelic research to the forefront. Publications like Third Wave are also critical in showcasing the most exciting neuroscience studies to date:
- For instance, Johns Hopkins Center for Psychedelic and Consciousness Research is leading the way in exploring innovative hallucinogenic treatments. Its Director, Roland R. Griffiths, PhD, has authored over 400 journal articles on the topic so far. In 2016, Griffiths conducted a smoking cessation study using psilocybin therapy with Cognitive Behavioral Therapy (CBT) and psychedelic integration. At the six-month mark, 80% of smokers in the pilot study had abstained from cigarettes for at least a week.
- The Multidisciplinary Association for Psychedelic Studies (MAPS), founded by Rick Doblin, has been integral in igniting the third psychedelic wave by sponsoring numerous FDA-approved clinical trials. MAPS’ Senior Medical Director, Michael Mithoefer, MD, has worked on phase 2 and phase 3 trials of MDMA-assisted psychotherapy and provided MDMA-assisted sessions for therapists who completed the MAPS training program.
- UCLA’s Lundquist Institute has been another formative organization leading the way in psychedelic research. The Institute’s investigator, Charles Grob, MD, conducted the first FDA-approved phase 1 study of MDMA, along with a multinational study of the Amazonian plant hallucinogen, ayahuasca, and a pilot study of effects of psilocybin therapy for cancer patients dealing with end-of-life anxiety.
- New York University Langone’s Center for Psychedelic Medicine encompasses another group of cutting-edge researchers. The brand-new center announced plans to support basic science as well as phase 3 clinical trials. Primarily, it will focus on psychiatry, medicine, and preclinical research. Plus, the Center will help train faculty members and postdoctoral fellows to become independent investigators in psychedelic therapy.
These organizations and the trailblazers who lead them are paving the future of legal psychedelic medicine. But as it stands today, ketamine is the only legally approved psychedelic therapy.
In 2020, Johnson & Johnson announced that it received FDA approval to manufacture SPRAVATO (esketamine), a ketamine-based nasal spray to treat depressive symptoms in adults with major depressive disorder (MDD) and suicidality. Since then, clinics all over the country began administering ketamine off-label via IV infusions, intramuscular injections, and sublingual dissolving tablets to create a multitude of mental health conditions.
Ketamine Therapy
Ketamine, at both low doses and psychedelic doses, has significant psychotherapeutic potential for treating pain, suicidality, PTSD, and depression. Fortunately, due to ketamine’s legal status, health professionals have sought training and participated in their own ketamine experiences to understand best practices for administration, dosing, preparation, integration, set and setting, and harm prevention.
Here’s what we know about ketamine’s therapeutic use today:
Dosing: In the JAMA Psychiatry journal, the authors agreed that administering a low dose of 0.5 mg/kg/hour for 40 minutes via IV is the most effective course of action. A few years after JAMA published this consensus, the University of Pennsylvania offered guidelines that suggested a slightly wider dosing variation of up to 1 mg/kg/hour.
Preparation: Ketamine is considered to be very safe, even for patients with a history of psychosis. But due to potential blood pressure and heart rate changes, practitioners should prepare to screen out high-risk candidates, monitor patients’ vital signs, and respond to possible adverse events.
In addition, psychedelic health professionals must prepare patients for the experience itself. According to observational accounts, people commonly feel anxiety and fear before ketamine infusions. That’s why it’s so essential for practitioners to inform patients about ketamine’s safety, what the journey feels like, and the importance of setting intentions.
Integration: Ketamine is known to be highly effective–at least in the short term. But research doesn’t necessarily prove its long-term benefits. To help solidify lasting well-being, practitioners are helping patients integrate the experience into their day-to-day lives. Follow-up integration practices such as psychotherapy, meditation, journaling, and breathwork can (and should) be used to instill enduring change. In fact, the Journal of Psychotherapy and Psychosomatics showed that Cognitive Behavior Therapy as a tool for ketamine integration could successfully prevent relapse in patients with treatment-resistant depression.
Set and setting: Set describes the patient’s mindset and mental health goals. Setting defines the actual location where the experience takes place and how it could accelerate or hinder the healing experience. A recent qualitative study of ketamine patients suggests that set and setting were highly influential in determining feelings of connection, meaning, mysticism, and transformation. This means ketamine treatment centers must balance the need to run a medical-grade facility with the patients’ needs for comfort. This may involve black-out eye masks, weighted blankets, soft reclining chairs, psychedelic music, and calming art.
Harm reduction. Not every ketamine experience is filled with proverbial rainbows and butterflies. In fact, some journeys may reveal darker aspects of the psyche that patients have suppressed. Patients may even experience nightmares or find themselves more anxious after psychedelic sessions. That’s why it’s critical to employ trained therapists to help patients navigate these experiences, make sense of the lessons they receive, and integrate them in a healthy way.
Incorporating this vast trove of experiential and clinical data is a great start, but it’s not enough on its own. According to JAMA’s consensus report, the medical community also needs to “develop a coordinated system of data collection on all patients receiving ketamine for the treatment of mood disorders. After such a registry is created, all clinicians providing ketamine treatment should consider participation.”

Maya’s Data-Driven Solution
As a team deeply rooted in psychedelic science and experiential wisdom, Maya agrees that the best way to advance the field is to gather knowledge, methodologies, and outcomes data from the psychedelic professional community. When practitioners, retreats, clinics, participants, and researchers can collaborate through Maya’s data-driven platform, they can co-create a map that leads to the most successful clinical outcomes.
Leveraging vast data on personal health and well-being, set and setting, preparation, and integration, clinicians can hold space to have the most significant impact on the countless people who’ve struggled and failed to find relief from traditional psychiatric medicine. Maya’s mission is clear:
“I believe we can harness the wisdom of the lineages and bridge the gap between theoretical research and real-world psychedelic practices. We can marry scientific rigor with intuition and cultural wisdom. We can collect the world’s cumulative knowledge and channel it towards a safe, expansive, and scalable future for psychedelic healing,” said David Champion, Maya’s CEO & Founder.
Maya has developed the technology that psychedelic healers need to comprehensively map patient care journeys, improve outcomes, and increase access to safe, standardized care to turn its beliefs into reality. The growing third wave can solidify into lasting change when the modern world develops a holistic knowledge base incorporating real-time data, historical wisdom, and critical patient (and practitioner) experiences.
If you are curious about joining the movement to map the psychedelic experience, Maya offers practitioners and clinics exclusive access to the platform before it’s available to the public. To redeem the limited-time offer, mention ThirdWave in “referrals” when you sign up.